Most people with pulmonary fibrosis will require supplemental oxygen, or oxygen therapy, at some point in their lifetime. If your condition is diagnosed very early, you may not require supplemental oxygen for some time. Some patients may require supplemental oxygen only while asleep or during exercise. Other patients may require extra oxygen nearly all the time.
1. Why you need supplemental oxygen
The scarring of pulmonary fibrosis inhibits your lungs’ ability to exchange carbon dioxide and oxygen from the air you inhale. Oxygen is vital for the proper functioning of all your organs, most importantly your brain and heart. If your lungs are not able to extract adequate oxygen on their own, you could suffer irreversible damage from low oxygen levels.
Some people are reluctant to use supplemental oxygen. They may fear becoming dependent or “addicted” to supplemental oxygen. But your lungs are not like muscles: you cannot recover your lung function after it has been damaged. Oxygen is more like high-octane fuel for your car. When you need more oxygen, use it.
As Baby Boomers age, more people are using medical devices in public. Using supplemental oxygen is not a sign of weakness. For the most part, people are friendly and, if they treat you differently, they are likely to be courteous and accommodating.
2. Oxygen therapy requires a prescription
A six-minute walk test measures your oxygen saturation during exertion. A healthcare professional uses a pulse oximeter to monitor your oxygen level and pulse rate as you walk at your normal speed for exactly six minutes. If your oxygen saturation drops below 88% during the test, it indicates that you need supplemental oxygen. In the United States, a six-minute walk test or similar documentation from a doctor is needed to justify insurance coverage to pay for your oxygen service.
Your doctor should also instruct you on when to use supplemental oxygen. Using supplemental oxygen during sleep is common. If you are using supplemental oxygen while sleeping, be sure you are using a device set on continuous flow for best results. Your doctor may say you need to use supplemental oxygen “on exertion.” This means that any time you are very active, exercising, doing heavy housework, gardening, and so on, you should use oxygen.
3. Insurance coverage for oxygen varies
In the U.S., patients most often rent oxygen equipment from a durable medical equipment (DME) provider. Medicare or other health insurance frequently cover the cost of basic equipment, if the patient is qualified. Your doctor’s office may recommend or choose a distributor for you. Rental agreements have “strings” attached, so be sure to read any agreement before signing. Your insurance company or Medicare may require a yearly test, usually a six-minute walk test, to continue paying for supplemental oxygen. They may also require documentation from your physician consistent with their requirements.
It is a good idea to review your health insurance policy to determine what type of oxygen therapy is included. You may have to pay a deductible or a co-pay, depending on your insurance coverage. Some insurance covers only a home concentrator and portable tanks for out of the home, but do not pay for a portable concentrator. Avoid nasty surprises by carefully checking your health insurance coverage in advance.
4. The numbers on portable oxygen devices are not Liters Per Minute
Your doctor will prescribe the level of supplemental oxygen you need. The level is prescribed in liters per minute (LPM) and typically is between 1 to 10 liters per minute, with 2 LPM being common at first. The LPM oxygen flow rate of 2 indicates that 2 liters of oxygen should flow into the patient’s nose in 1 minute.
The most important thing to know is that your portable oxygen device has numbers on it dial. But these numbers do not mean liters per minute. They are settings, more like low, medium, and high. Most portable devices do not delivery oxygen continuously, but are triggered when you inhale, called pulse mode. At it highest setting, portable oxygen concentrators that are light enough to carry will not deliver more than 1 – 2 liters per minute. If your doctor prescribes 2 LPM, you may need to set your device at its highest setting and it still may not be enough to keep your saturation level in a healthy range. Always rely on your pulse oximeter to determine if you are getting adequate oxygen.
5. Monitor oxygen level with an oximeter
Physical activity can temporarily decrease your oxygen level. Your oxygen level will also vary with other factors, including how frequently and how deeply you breathe. You do not always notice when your oxygen level is low. That is why it is important to have a way to monitor yourself during daily activities, even when using supplemental oxygen.
Use a pulse oximeter to measure your blood oxygen level at home. The oximeter comfortably fits over one of your fingertips and reads your pulse rate and your blood oxygen saturation, which is the percentage of oxygen in your blood. The healthy range for an oxygen reading is 95 to 100%. Readings between 90 and 95 are tolerable for patients with lung disease. Readings below 88 – 90 indicate that too little oxygen is available for your body to function normally. It is time to use your supplemental oxygen to raise your saturation.
You can buy a pulse oximeter at pharmacies or big box stores for twenty to fifty dollars (USD). They are accurate for home and gym use. Most oximeters are accurate to within 2 to 3 percentage points. You can take your device with you to your doctor’s office and compare its reading with that of the device your doctor uses. Other, more accurate devices are available at a higher cost.
6. Oxygen comes in many forms
There are many forms of supplemental oxygen delivery systems including oxygen tanks, home concentrators, portable oxygen concentrators (POC), and liquid oxygen.
Oxygen tanks provide highly compressed oxygen directly to your nose. Oxygen tanks come in a variety of sizes. Some tanks are portable and can be carried in a shoulder bag or mounted on a cart to be pulled or pushed. Depending upon the type of control regulator used, tanks can be low flow (.5 to 5 LPM) or high flow (.5 to 15 LPM).
The durable medical equipment provider (DME) can provide filled tanks and replace used tanks. Some providers will give the patient a home fill unit where tanks can be filled by the user.
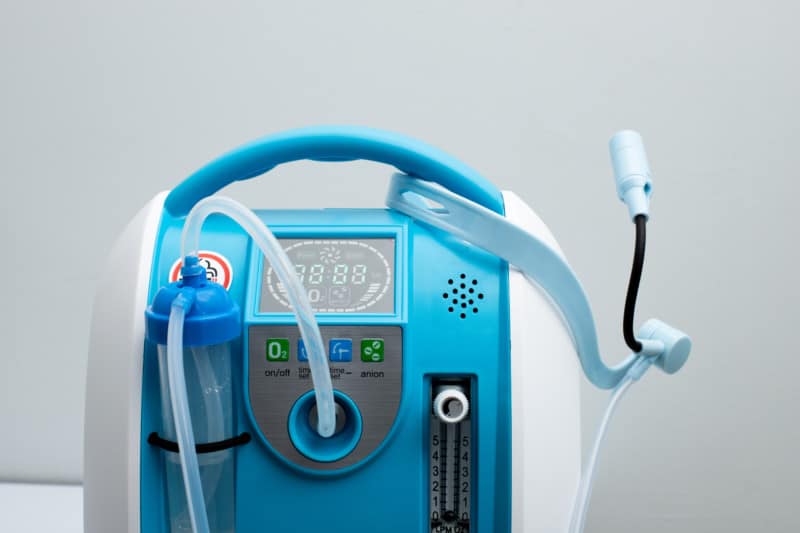
Oxygen concentrators remove the nitrogen in the ambient air and thus deliver almost pure oxygen. Home oxygen concentrator units can operate 24 hours per day from a common electric outlet. They weigh about 40 pounds and have rollers for moving the unit. They come in either low flow or high flow units.
Portable oxygen concentrators are battery-powered and weigh about up to 20 pounds. The smaller portable units deliver only about 1 LPM in a pulse flow, and if this is high enough for you, it allows you to get out and be more active.
Larger portable units are available that are heavier (around 18 to 20 lbs.). Most of these types can deliver 3 LPM on constant flow and some may deliver up to 5 LPM with conserving settings. They usually need to be carried on a cart due to weight. Constant flow will provide higher LPM, but batteries will not last as long.
For patients who require higher flow, liquid oxygen is a solution that can deliver a higher flow and a longer-lasting supply. Liquid oxygen can be difficult to obtain due to regulations for insurance reimbursement. Many DMEs choose not to provide liquid oxygen because of the difficulty.
7. Plan ahead to travel with oxygen
Traveling with oxygen takes a bit of planning to be sure you are doing so safely.
For air travel, airlines may require you to complete a form and give a doctor’s letter to allow you to carry on a portable oxygen concentrator. Airlines and some cruise lines prohibit oxygen tanks. Airlines typically pressurize cabins to around 8,000 feet elevation. So, you may need a higher flow of supplemental oxygen than you do at sea level. Check that your portable oxygen concentrator will be able to meet your needs.
The battery life of your POC is important. Most airlines require you to carry batteries to provide power at least 1½ times the expected length of the flight. Check with airlines a few weeks before travel to comply with their regulations.
For travel by car, newer POCs allow you to recharge in an electrical outlet or in most cars. Users should take extra batteries, a car charger, and a power supply (like the one for portable computers) with them when going out or traveling.
At higher altitudes your body will require more supplemental oxygen that at sea level or your usual altitude. Plan to use more oxygen at higher delivery levels than normal. You may ask your doctor if you should be tested before traveling to see what level of oxygen will suffice.
Summary
Supplementary oxygen provides the vital breath of life for those with pulmonary fibrosis. Portable tanks or portable oxygen concentrators can allow you to go out, travel, exercise and do the things you love. it will just take a bit of getting used to.
Watch a PF Warriors meeting replay Respiratory Therapy and Oxygen .